Hip Arthroscopy in Sports Medicine: Indications and Outcomes
Hip arthroscopy has emerged as a critical procedure in sports medicine, offering minimally invasive options for treating various hip conditions. This technique allows surgeons to visualize, diagnose, and treat issues within the hip joint without the need for extensive open surgery. Athletes suffering from hip pain caused by injuries, labral tears, or femoroacetabular impingement can benefit significantly from this procedure. The primary indication for hip arthroscopy includes conditions that do not respond to conservative management. Prominent indications encompass labral tears, synovitis, cartilage damage, and loose bodies in the hip joint. In young athletes, particularly, early intervention can prevent further joint degeneration, leading to improved long-term outcomes. While hip arthroscopy is considered safe, like any surgical procedure, it carries inherent risks, such as infection, nerve injury, and persistent pain. Successful outcomes heavily rely on proper patient selection, preoperative assessment, and postoperative rehabilitation. In addition, the clinician’s skill greatly influences postoperative recovery and ultimate performance return. For athletes, returning to their sport after surgery typically depends on both the type of injury and the effectiveness of postoperative rehabilitation. Such tailored protocols ensure optimal recovery and performance.
Common Indications for Hip Arthroscopy
Among the common indications for performing hip arthroscopy in athletes, labral tears stand out. A labral tear occurs when the cartilage ring surrounding the hip socket becomes damaged, often due to repetitive stress or acute trauma. These tears can result in pain, limited range of motion, and mechanical symptoms such as clicking or locking sensations. Another significant indication is femoroacetabular impingement, characterized by abnormal bone growth influencing joint movement. This condition can interact with hip mechanics and potentially lead to premature osteoarthritis. Synovitis, inflammation of the synovial membrane, may also warrant arthroscopic intervention, as chronic inflammation can perpetuate pain and dysfunction. Loose bodies, which are fragments of cartilage or bone floating within the joint, can cause mechanical problems and intense discomfort, necessitating their removal. Each of these conditions not only affects athletes’ performance but can also incur long-lasting hip issues if left untreated. Furthermore, hip arthroscopy allows for diagnostic confirmation of these issues through direct visual inspection during the procedure. To summarize, recognizing these indications early can facilitate timely treatment and enhance athletes’ quality of life and competitive longevity.
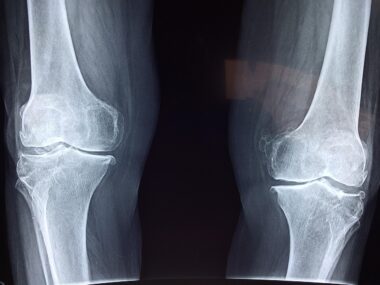
Preoperative assessment plays a vital role in the successful implementation of hip arthroscopy. A thorough evaluation includes a detailed history, physical examination, and advanced imaging. This comprehensive approach aims to determine the extent of the injury and assess key factors affecting surgical success. Magnetic resonance imaging (MRI) is commonly employed to visualize the joint structures clearly and identify potential conditions. MRI can reveal labral tears and cartilage defects, guiding surgical planning. Following diagnostics, preoperative education is essential, as it equips patients with realistic expectations regarding the recovery process and potential outcomes. Surgeons must communicate the procedure’s benefits and possible complications effectively. Moreover, patient-centered approaches to care ensure that athletes remain engaged in the treatment process. Patients should actively participate in their rehabilitation planning, aligning recovery with their personal goals, whether that is returning to competitive sports or daily activities. Establishing a clear understanding of the rehabilitation protocol forms the foundation for postoperative success. In conclusion, proper preoperative management sets the stage for achieving optimal surgical outcomes while fostering a strong patient-surgeon rapport.
The Procedure: Steps and Techniques
The hip arthroscopy procedure typically involves several steps, utilizing advanced equipment to minimize invasiveness and enhance visualization. Initially, the patient is positioned to ensure optimal access to the hip joint. Anesthesia, either general or regional, is administered before the procedure begins. The surgeon then makes small incisions, called portals, around the hip, through which specialized instruments are inserted. A camera helps provide a high-definition view of the joint, allowing for detailed visualization of the intra-articular structures. As the surgeon inspects the joint, they can perform specific interventions, such as labral reconstruction, cartilage repair, or synovectomy, based on findings. Furthermore, these techniques allow for flexible approaches, minimizing tissue trauma while maximizing repair capabilities. Throughout the procedure, surgeons continually evaluate the joint for abnormalities and address issues as they arise. Postoperatively, patients are monitored for any potential complications, and pain management strategies are implemented. The overall goal is to ensure both immediate and long-term success through careful procedural adherence. Successful execution of hip arthroscopy hinges on surgical precision, advanced training, and an in-depth understanding of anatomical structures.
Postoperative Management and Rehabilitation
Postoperative management plays a critical role in achieving the best outcomes after hip arthroscopy. Effective pain control is necessary for promoting early mobility and initiation of rehabilitation exercises. Professionals often prescribe medications, including analgesics and anti-inflammatories, tailored to individual needs. Incorporating physical therapy shortly after surgery is vital to prevent stiffness, improve range of motion, and rebuild strength. A structured rehabilitation program will typically progress through phases, starting with gentle range of motion exercises and gradually introducing strength and functional training as healing allows. Patients and therapists work together to set specific goals throughout the recovery process. Furthermore, compliance with rehabilitation protocols significantly influences the recovery timeline and performance experiences. Significantly, the rehabilitation phase can take anywhere from a few weeks to several months, depending on the extent of the surgery and the initial condition. Moreover, maintaining open communication with healthcare teams ensures that any emerging issues are addressed promptly. Establishing a solid connection and supportive environment fosters patients’ mental well-being, which plays a lead role in successful recovery.
With advancements in surgical techniques and technology, the outcomes for athletes undergoing hip arthroscopy have improved considerably. Studies indicate that many players return to their pre-injury levels of competition, thus enhancing overall satisfaction and quality of life. Generally, those without significant pre-existing joint damage tend to experience more favorable outcomes, highlighting the importance of early intervention. Patients and surgeons alike must maintain realistic expectations regarding recovery timelines and potential risks. While a large percentage of athletes successfully regain their functionality, some may continue to experience residual pain or mechanical symptoms. Monitoring patients during follow-up visits ensures that practitioners can swiftly address any concerns promptly. Furthermore, it allows for tailored adjustments in rehabilitation protocols based on individual performance and needs. Evidence suggests that dedicated rehabilitation efforts directly correlate with improved outcomes, emphasizing the necessity of structured intervention post-surgery. Ultimately, the benefits of hip arthroscopy should be weighed against potential risks, ensuring that athletes receive comprehensive guidance to make informed decisions about their treatment. Overall, ongoing research and advancements promise to further refine the results following hip arthroscopy.
Conclusion
In conclusion, hip arthroscopy is a valuable tool in sports medicine, addressing various hip conditions through minimally invasive methods. With careful consideration of indications, thorough preoperative assessments, and organized postoperative rehabilitation, athletes can achieve significant improvements and return to their beloved sports. The combination of technical advancements in the surgical field and enhanced understanding of rehabilitation techniques contributes to successful outcomes. Athletes who experience hip issues should engage with their healthcare providers to explore surgical options, ensuring their recovery aligns with their personal goals. As sports medicine continues to evolve, future innovations will certainly provide further enhancements to patient outcomes following hip arthroscopy. Engaging in dialogue with a multidisciplinary team fosters a collaborative approach, ultimately leading to comprehensive patient care. Moreover, continuous research into the long-term effects of hip arthroscopy is integral to building foundational knowledge, driving further progress in this area. Overall, hip arthroscopy is a promising and effective strategy for addressing hip-related issues among athletes, warranting its ongoing importance in sports medicine practice. With balanced expectations and commitment, both patients and healthcare teams can optimize results and encourage long-lasting health in active individuals.
Hip Arthroscopy in Sports Medicine: Indications and Outcomes
Hip arthroscopy has emerged as a critical procedure in sports medicine, offering minimally invasive options for treating various hip conditions. This technique allows surgeons to visualize, diagnose, and treat issues within the hip joint without the need for extensive open surgery. Athletes suffering from hip pain caused by injuries, labral tears, or femoroacetabular impingement can benefit significantly from this procedure. The primary indication for hip arthroscopy includes conditions that do not respond to conservative management. Prominent indications encompass labral tears, synovitis, cartilage damage, and loose bodies in the hip joint. In young athletes, particularly, early intervention can prevent further joint degeneration, leading to improved long-term outcomes. While hip arthroscopy is considered safe, like any surgical procedure, it carries inherent risks, such as infection, nerve injury, and persistent pain. Successful outcomes heavily rely on proper patient selection, preoperative assessment, and postoperative rehabilitation. In addition, the clinician’s skill greatly influences postoperative recovery and ultimate performance return. For athletes, returning to their sport after surgery typically depends on both the type of injury and the effectiveness of postoperative rehabilitation. Such tailored protocols ensure optimal recovery and performance.